Merkel Cell Carcinoma FAQs
What is Merkel cell carcinoma? »
 Also known as neuroendocrine carcinoma of the skin, Merkel cell carcinoma is a rare type of skin cancer. It occurs in the Merkel cells, which are found at the base of the epidermis, the skin’s outermost layer.
Also known as neuroendocrine carcinoma of the skin, Merkel cell carcinoma is a rare type of skin cancer. It occurs in the Merkel cells, which are found at the base of the epidermis, the skin’s outermost layer.
It usually appears as flesh-colored or bluish-red nodules on the face, head, or neck. This form of skin cancer metastasizes quickly. It also has a high incidence of recurring.
How is Merkel cell carcinoma diagnosed? »
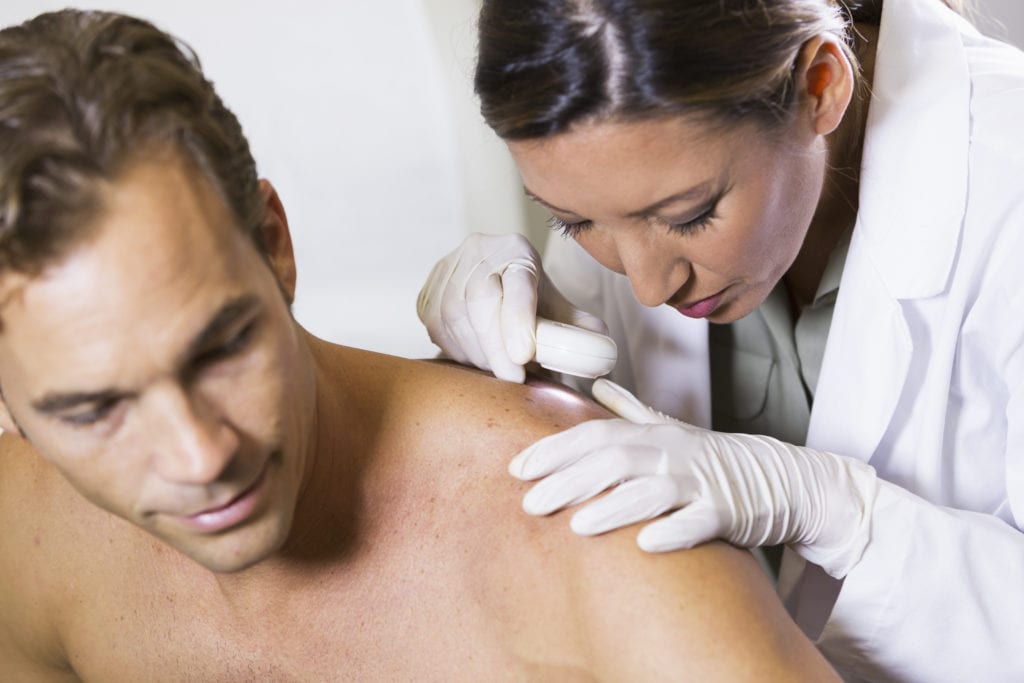
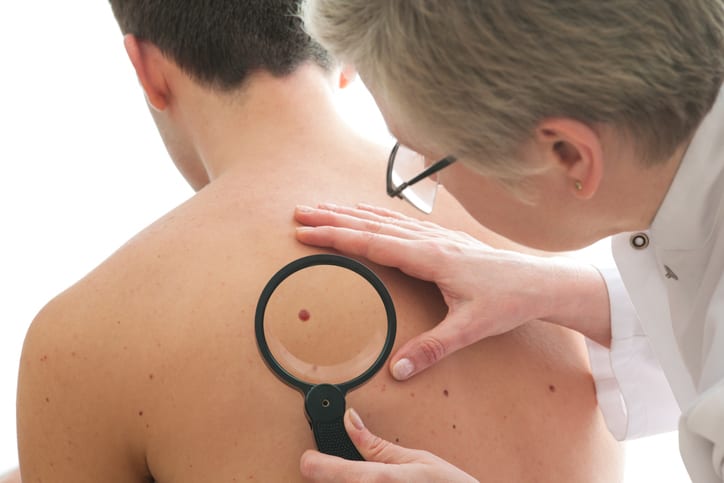
With Merkel cell carcinoma, early diagnosis is key to successful treatment. This includes self-diagnosis. The American Cancer Society recommends that adults check their skin once a month. You should have a general idea of your patterns of moles, blemishes, freckles, and other marks on your skin. That way you can look for changes. You need to examine all of your skin, including your palms and soles, scalp, ears, nails, and your back. Have a friend or partner check your back and scalp.
You’re looking for any skin changes. If you notice any spots on your skin that are new or changing in size, shape, or color you need to see a dermatologist immediately.
Seeing a dermatologist once a year should be a part of your healthcare regimen. This is particularly true after you turn 40 (earlier if you’ve had lots of sun exposure). A biopsy of your skin growth will usually be the confirmation of Merkel cell carcinoma.
How is Merkel cell carcinoma different from other skin cancers, such as basal cell carcinoma? »
Merkel cell carcinoma is much less common than most the other types of skin cancer, but it, along with melanoma, is one of the most dangerous types. When compared to basal cell and squamous cell skin cancers, Merkel cell carcinoma is much more likely to spread to other parts of the body. Once this happens, odds of successful treatment drop dramatically.
What does Merkel cell carcinoma look like? »
These cancers most often start on the typical areas that receive lots of sun exposure — the face (this is the most common site), neck, and arms. They can form anywhere on the body, however. Merkel cell tumors usually look like firm, pink, red, or purple lumps or bumps on the skin.
What causes Merkel Cell carcinoma? »
The causes of Merkel cell carcinoma are not fully understood. The Merkel cells are connected to the nerve endings in the skin that are responsible for the sense of touch. Recent research points to a common virus that likely plays a role in development of this rare skin cancer, the Merkel cell polyomavirus. This virus lives on the skin and doesn’t have any symptoms and is very common. It’s not clear why it sometimes may cause this rare skin cancer.
 These are thought to be the risk factors for Merkel cell carcinoma:
These are thought to be the risk factors for Merkel cell carcinoma:
- Excessive UV exposure
- A weakened immune system
- History of other skin cancers
- Being over age 50
- Light skin color
What are the symptoms of Merkel cell carcinoma? »
Merkel cell carcinoma usually starts on areas of skin exposed to the sun, especially the face, neck, arms, and legs. It first appears as a single pink, red, or purple shiny bump that doesn’t hurt. These can bleed at times.
These tumors grow quickly, and they can form new lumps near the first location. They can spread to nearby lymph nodes. If this happens the lymph nodes can grow so that they become visible as lumps under the skin. This usually occurs in the neck or under the arm.
Merkel cell carcinoma is rare, and the first signs of it can look like more common forms of skin cancer that aren’t as aggressive. That makes early detection critical, as in many cases only a biopsy will identify it as Merkel cell carcinoma.
How Common is Merkel Cell Carcinoma? »
This type of skin cancer is very rare. Doctors diagnose only about 3,000 cases each year. In recent years, we’ve seen an increase in diagnoses. This could be due to greater awareness about skin cancer among patients and doctors and also more advanced diagnostic screenings for abnormal skin cells.
Can Merkel Cell Carcinoma be Prevented? »
There are several steps that can be taken to reduce the risks of developing Merkel cell skin cancer. These are the same steps you’d take to protect yourself from the more commonly known skin cancers, basal cell carcinoma and squamous cell carcinoma. While there are other factors that can contribute to the risk of Merkel cell carcinoma, including age and lowered immunity, sun exposure continues to be one of the primary factors across the board. To keep yourself as safe as possible, it’s important to avoid excessive sun exposure, wear broad-spectrum SPF 30 sunscreen every day, avoid tanning bed use, and wear protective clothing like a wide-brimmed hat on particularly sunny days or on days you’ll be outdoors for more than an hour or two.
Melanoma has the Highest Mortality Rate of All Skin Cancers. Why is Merkel Cell Carcinoma Considered More Dangerous? »
Merkel cell carcinomas are very rare. Not much is known about this rare form of skin cancer, especially in comparison to melanoma. People tend to know what to look for to assess their skin for melanoma (ABCDE). Because of this, most melanomas are identified at stage 0, the in situ stage where the growth has not invaded deeper layers of tissue and there is very little risk of metastasis. There is little awareness about Merkel cell carcinoma so most people don’t even know what to look for. Furthermore, the early signs of Merkel cell carcinoma are inconspicuous. These growths rarely look concerning so aren’t evaluated until they’ve grown to become cosmetically obvious. At that point, there is a higher likelihood of metastasis to lymph nodes or periphery areas of the body. In fact, doctors may perform tests on nearby lymph nodes for a Merkel cell carcinoma as small as four or five millimeters. There is a 15 percent chance that a growth of this size has spread to the lymph nodes or farther.
How Can People Spot Merkel Cell Carcinoma Before Cancer can Spread to Nearby Lymph Nodes or Beyond? »
We can’t spot Merkel cell carcinomas in the same way we’ve come to identify melanoma or other common skin cancers. Instead of ABCDE, these lesions are best found through AEIOU. Often the earliest Merkel cell carcinomas are Asymptomatic! However, they may Expand at a rapid pace. Merkel cell carcinoma is more common among the Immunocompromised and in people Older than age 50. Finally, exposure to Ultraviolet light is a factor to consider when looking for signs of Merkel cell carcinoma. According to studies, nearly 90 percent of patients diagnosed with this rare skin cancer exhibit at least three of the AEIOU characteristics. While these characteristics are not 100 percent indicative of Merkel cell carcinoma, they are sufficient to warrant a thorough clinical exam of a suspicious growth.
How is Merkel cell carcinoma treated? »
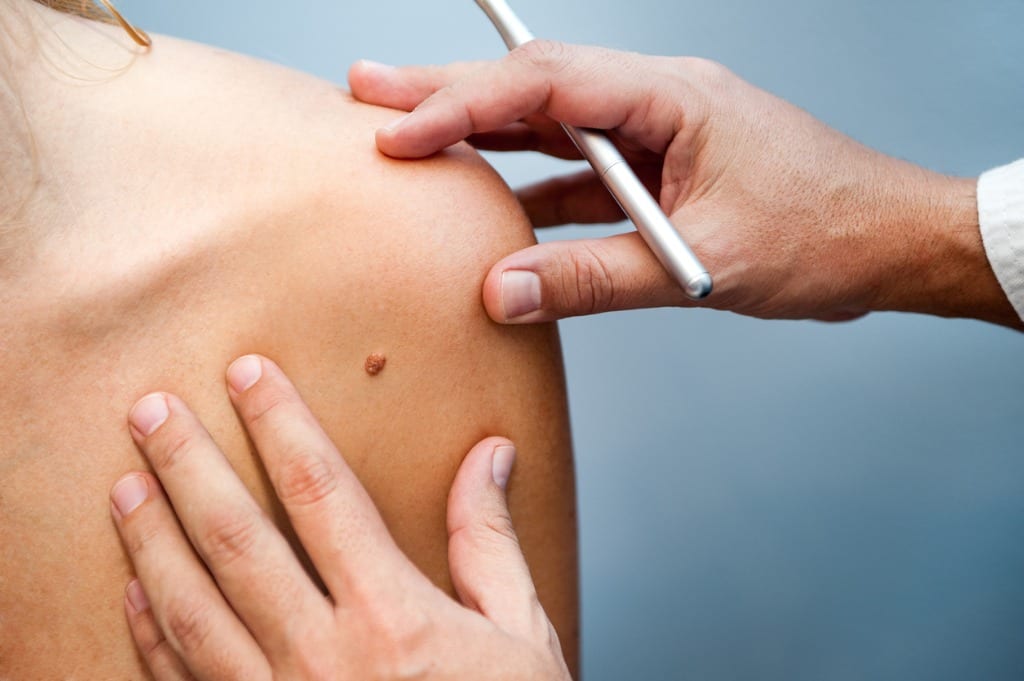
Excision is the first treatment option for Merkel cell carcinoma. The tumor along with a border of normal skin is removed. This may be done with a standard scalpel excision or it may be done with Mohs surgery to limit the amount of healthy tissue removed and manage future scarring.
If the cancer has spread to the lymph nodes, they will be removed in what is called lymph node dissection.
If the cancer has spread to other parts of the body, the treatments may include radiation therapy, immunotherapy, or chemotherapy.
“The ASMS is an outstanding resource to learn about Mohs surgery both for patients, physicians, and technicians. The society is committed to improving the care of patients and the skill sets of doctors and technicians performing Mohs surgery.” – A.G.
What is the cure rate of Merkel cell carcinoma? »
As with melanoma, early diagnosis of Merkel cell carcinoma is imperative to increase the patient’s odds of successful treatment.
The five-year survival rate for localized Merkel cell carcinoma, meaning it has not spread, is 78%. If the cancer has spread to the lymph nodes or other nearby structures, the five-year survival rate is 51%. If it has spread to distant organs or parts of the body, the five-year survival rate is just 17%

Are there risk factors for developing Merkel cell carcinoma? »
- Merkel cell polyomavirus infection — This virus was first discovered in 2008, and it’s still somewhat of a mystery. This virus is found in the cancer cells of 80 percent of people with Merkel cell carcinoma.
- UV light exposure — Exposure to the ultraviolet rays is the major risk factor (as with all skin cancers). This exposure can come from the sun, tanning beds, or from UV light treatments for psoriasis.
- Fair skin — Nearly 90 of Merkel cell carcinomas occur in white people.
- Old age — This form of skin cancer is very rare in people under the age of 50. Over 80 percent of cases form in those over 70. This is probably due to a combination of accumulating UV exposure and a weakening immune system.
- Males — Men are twice as likely to get this skin cancer, although again that can simply be a factor that men get more sun exposure.
- Weakened immune system — Our immune systems not only fight germs and viruses, they also help the body fight cancer. When these systems are weakened, the patient becomes more likely to develop some types of cancer, including Merkel cell carcinoma.
What is the prognosis for Merkel cell carcinoma? »
You can see the cure rate for this type of skin cancer in the adjacent section. This is a rare and very dangerous form of skin cancer. Successful prognosis invariably involves early detection. Almost 80 percent of cases found early have good five-year success rates. But if the cancer has spread to the lymph nodes and to other parts of the body, the prognosis is not good.
That’s why it’s important for you to regularly check your own skin and have an understanding of the growths, freckles, and the like on it. If you don’t see a dermatologist regularly, you need to do so. Find one and see them once a year.
Learn More About Merkel Cell Carcinoma Today »
If you’re interested in learning more about Merkel cell carcinoma, please click the button below to find a Mohs Surgeon near you.


