Melanoma FAQs

What is melanoma Skin Cancer? »
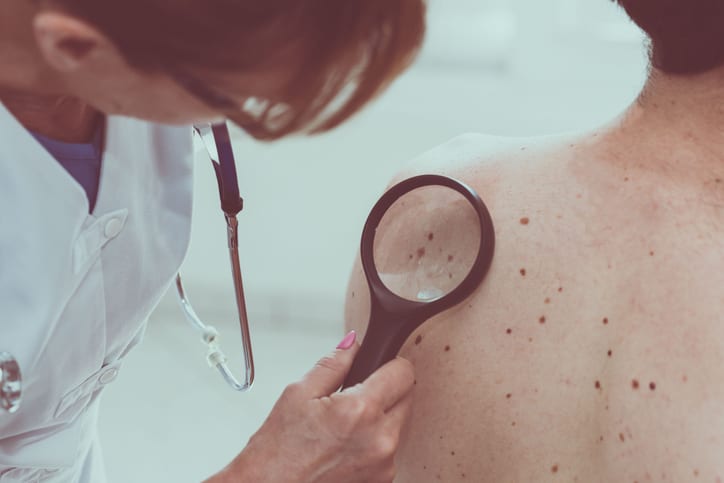
Melanoma is the most dangerous type of skin cancer. It develops in the skin cells that produce melanin, the melanocytes. Exposure to ultraviolet radiation from the sun or from tanning beds increases a person’s risk of developing melanoma. The reason melanoma is more deadly than squamous cell or basal cell carcinoma is that as melanoma progresses it grows downward and can begin to deposit cancerous cells into the bloodstream where they can spread cancer anywhere in the body.
What causes melanoma? »
The exact causes of melanoma are not fully understood, as it can occur in both people who have had serious sun exposure (in those areas) and in those who have not (when it occurs on areas such as the soles of the feet). It occurs when the DNA of the melanin-producing cells, the melanocytes, is damaged. This causes these skin cells to grow out of control, which can eventually become a mass of cancerous cells.
It is believed that UV radiation is the leading cause. Melanoma is more common in those with fairer skin, as they have less melanin in the skin, which acts as a protection mechanism by darkening with sun exposure (tanning). It is thought that extreme peeling sunburns when a person is a child or adolescent have a direct correlation with an increased risk of melanoma. Research has shown that every one of these peeling sunburns can double the person’s risk of developing melanoma as an adult.
What are the symptoms of melanoma? »
Melanoma can develop anywhere on the body, but in fair-skinned people, it usually develops in areas that have had lots of sun exposure: the face, arms, back, and legs. Unlike other skin cancers, melanoma can also develop in areas that don’t receive sun exposure, such as the soles of the feet, the beds of the fingernails, and the palms of the hands. This is rarer and occurs most often in people with darker skin tones.
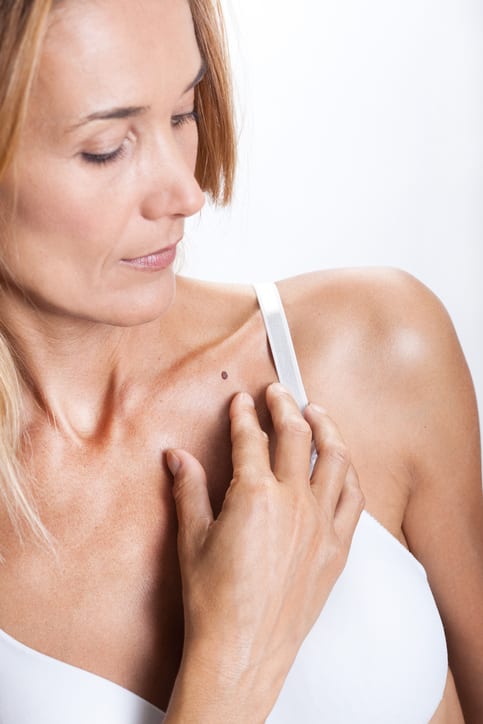 Melanoma is more common in people with over 50 moles on their body.
Melanoma is more common in people with over 50 moles on their body.
The first signs and symptoms of melanoma are:
- A change in an existing mole
- Development of a new pigmented or unusual-looking growth on your skin or area of your skin
This is not always the case, as melanoma can occur on skin that appears to be normal.
When considering a mole to be melanoma, it helps to remember these ABCDE warning signs:
- Asymmetry — If one half of the mole doesn’t match the other half, that’s a concern. Normal moles are symmetrical.
- Border — If the border or edges of your mole are ragged, blurred, or irregular, it should be checked.
- Color — Normal moles are a single shade throughout. If your mole has changed color or if it has different shades of tan, brown, black, blue, white, or red, then it should be checked.
- Diameter — If a mole is larger than the eraser of a pencil, it needs to be checked.
- Evolving — If a mole evolves by shrinking, growing larger, changing color, itching or bleeding, or other changes, it should be checked. Melanoma lesions often grow in size or gain height rapidly.
What are the types of melanoma? »
Most people assume there is just “melanoma.” There are actually four different types of this most dangerous form of skin cancer.
- Superficial spreading melanoma — This is the most common form. It can arise in an existing mole or appear as a new lesion. When it forms in a mole already on the skin, it tends to grow on the surface for a period of time before penetrating more deeply. It is most likely to occur on the torso in men, the legs in women, and the upper back in both sexes. Superficial spreading melanoma appears as flat or slightly raised and discolored, asymmetrical patches with uneven borders.
- Lentigo maligna — This form of melanoma often develops in older people. It also grows close to the surface skin in the beginning. This form typically develops on sun-damaged areas of the face, ears, arms, and upper torso. Lentigo maligna appears as flat or slightly raised, blotchy patches with uneven borders.
- Acral lentiginous melanoma — This is the most common form of melanoma found in people with darker skin tones, including those with African ancestry. It often forms in areas that are not easy to spot — under the fingernails or toenails, on the soles of the feet, or on the palms of the hands. It appears as a black or brown area.
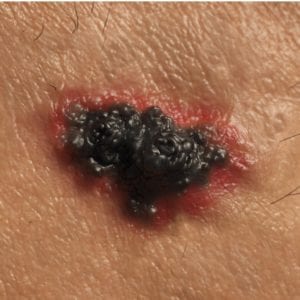
- Nodular melanoma — This is the most aggressive type of melanoma. It makes up 10-15 percent of all cases. These tumors grow deeper into the skin more rapidly than other types of melanoma. They are invasive tumors, meaning they’re likely to already have reached the deeper layer of skin by the time it is diagnosed. These are found most frequently on the torso, legs, and arms, and on the scalp in older men. These appear as a bump on the skin, usual blue-black in color.
How is melanoma treated? »
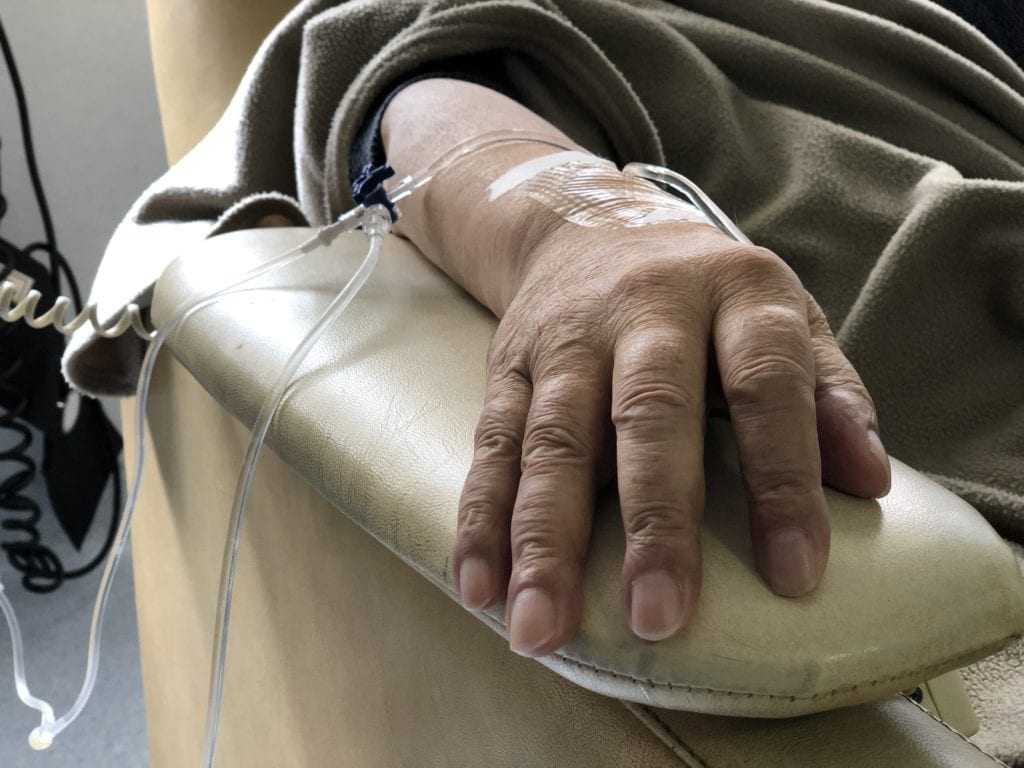 The treatment of melanoma depends on the size and stage of cancer. If caught early, melanoma can be fully removed during the biopsy. This is especially true if cancer has not started growing downward yet.
The treatment of melanoma depends on the size and stage of cancer. If caught early, melanoma can be fully removed during the biopsy. This is especially true if cancer has not started growing downward yet.
There has been some success with early-stage melanoma using medications that make the body attack the area with white blood cells. Lotions are applied to the area with the melanoma and they inflame the area to a degree that the skin almost becomes an open sore. This inflammation activates the white blood cells to hunt for invaders, killing the cancer cells.
Mohs surgery is effective for removing melanoma that has been diagnosed but hasn’t spread. Mohs surgery involves removing the melanoma and a surrounding ring of tissue. This outer ring is instantly examined under a microscope to see if there are cancer cells still present. If there are, another ring of tissue is immediately removed and examined. This process is repeated until the tissue is free of cancer cells. For Mohs surgery, you need to be sure to have a surgeon who is a member of the American Society for Mohs Surgery.
These methods are used to remove melanoma that has not spread. If the melanoma has spread, treatment for this skin cancer is similar to treatment for other cancers:
- Surgery to remove the affected lymph nodes
- Chemotherapy
- Radiation therapy
- Immunotherapy
What Treatment Options Are available for Advanced Cases of Melanoma? »
If a patient’s melanoma has spread beyond the surface skin, treating it is more difficult. Here are some methods and what is involved.
- Surgery to remove affected lymph nodes — This surgery, clinically known as lymphadenectomy, is done to remove melanoma that has spread only to the lymph nodes. This can prevent it from spreading to other areas of the body.
Since the lymph nodes usually affected by melanoma are near the surface of the skin, this is not a difficult surgery or recovery. If the lymph nodes in question are located in more difficult areas to access, recovery correspondingly will be more involved. Lymphedema may develop after the removal of the lymph nodes. This is an accumulation of lymphatic fluid that collects in the area where the lymph nodes were removed.
- Chemotherapy — Because chemotherapy uses drugs that course through your entire body to get to the cancer cells, it usually is not the best treatment for isolated melanoma. These drugs can damage your nerves and cause pain, burning, tingling, or weakness and sensitivity to hot and cold. Other side effects include hair loss, mouth sores, infection, and bruising or bleeding.
- Radiation — In advanced melanoma, radiation may be used to kill any cancer cells that may have been left behind after surgery or if the melanoma has spread to the brain or the bones.
- Immunotherapy — In Immunotherapy drugs help your immune system find and attack the cancer cells. Often patients are given more than a single drug, as this seems to cause fewer side effects. Sometimes these drugs can cause the immune system to attack healthy organs.
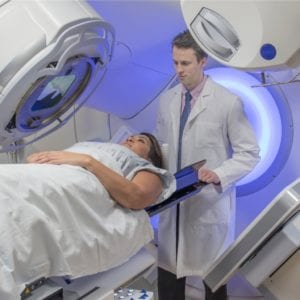
What are The Side Effects of Advanced Melanoma Treatment Options? »
Besides surgery, these other three treatments don’t have much “recovery” per se after the therapy is complete. However, they all have a similar set of side effects:
- Fatigue
- Appetite changes
- Constipation or diarrhea
- Itching
- Rashes
What is the cure rate for melanoma? »
If caught early, the success rate for treating melanoma is very high. That’s why yearly skin cancer screenings are so important, particularly for people with fair skin. The estimated five-year survival rate for patients whose melanoma is detected early is about 99 percent in the U.S. But when cancer has spread to the lymph nodes, the five-year survival rate falls to 63 percent. If cancer has spread to distant organs, this rate falls to just 20 percent.
Can melanoma appear suddenly? »
Yes. Sometimes an existing mole suddenly changes. Other times an area that appears as simple sun-damaged skin changes. Fortunately, when these are spotted during your regular visits to your dermatologist they can be effective, and usually successfully, treated.
Acral lentiginous melanoma and nodular melanoma can appear suddenly. Acral lentiginous melanoma may be visible, but the person may assume it is nothing more than a bruise on the foot or under a nail. Nodular melanoma will suddenly appear as a bump on the skin. Unfortunately, at this point, the melanoma has usually grown deeper in the skin.
Can melanoma lead to other cancers? »
The research on this is not extensive, but studies have pointed to a link. The biggest risk for patients who have had a previous melanoma that was treated and removed is to develop another melanoma. The risk for patients who had a previous melanoma for developing a second case is nine times greater than the general population’s risk of developing melanoma.
There is also an increase in other cancers. The most common second cancers after a person have had melanoma were breast, prostate, and non-Hodgkin’s lymphoma.
What are the risks of melanoma treatments? »
There is little to no risk for the early treatment of melanoma. In fact, early treatment has a 99 percent five-year survival rate in the U.S. The real risk is not being checked for skin cancer and, as a result, not treating it. When cancer has reached the lymph nodes, the survival rate drops to 63 percent, 20 percent when it spreads to distant organs.
Learn More About Melanoma Today »
If you’re interested in learning more about melanoma, please click the button below to find a Mohs Surgeon near you.


